Families Disclosure of Mental Illness Soap Note Example.

The notes y'all accept equally a behavioral health care professional make up one's mind the quality of care your patients receive. Having notes that are comprehensive yet curtailed, and informative yet easy for other professionals to use is a skill that ofttimes takes years to master.
Using a pre-adamant framework in your patient notes can assist you meliorate the quality of your documentation.
I of the more than popular methods for creating documentation is to take SOAP notes. The four-pronged approach of SOAP notes was developed using the principles of thetrouble-oriented medical record (POMR) pioneered past doc Lawrence Weed.
In its early days, the Lather method was used only by medical professionals. Today, it's recognized as an effective communication tool between health care providers of all disciplines to document a patient'southward handling.
Table of Contents
- What Are SOAP Notes and How Do I Write Them?
- Why SOAP Notes Are an Important Tool
- Examples of Lather Notes
What are Soap Notes and How Do I Write Them?
The SOAP framework includes four critical elements that represent to each letter in the acronym — Southwardubjective, Objective, Assessment, and Plan.
These four stages offer an ideal standard for providing information necessary for all types of medical and behavioral wellness professionals to interact successfully with the notes.
Permit'southward examine each category in detail and drill downward on what you need to include in a SOAP note.

ane. Subjective
The first step is to gather all the information that the client has to share about their own symptoms. The patient will tell yous about their feel with the symptoms and condition, as well as what they perceive to be their needs and goals for handling.
It's crucial to record the patient'due south own words rather than paraphrasing them so y'all cultivate the well-nigh authentic insight into their status.
The Subjective category is also an appropriate place to list whatever comments made past the patient, their family unit members, or their caretakers.
This category is the basis for the residue of your notes as well as your handling programme, so getting the virtually quality information possible is paramount.
The Quondam CHARTS acronym provides a smart manner to cover a patient's condition systematically:
- Onset:Decide when each symptom first started.
- Location:Observe out the main location of pain or discomfort.
- Duration:Learn how long the patient has dealt with their symptoms.
- CHaracter: Examine the types of pain — aching, stabbing, etc.
- Alleviating or Aggravating Factors: What actions or interactions reduce or increase the severity of the patient's symptoms?
- Radiation: Find out if the pain radiates to other locations in the torso.
- Temporal Design: Practice the symptoms announced in a pattern like in the evenings or after meals?
- Southwardymptoms Associated: Are in that location any secondary symptoms that accompany the patient's chief complaint?
With the customer's symptoms fully documented, you can move to the adjacent portion of the notation.
2. Objective
The patient's experience is central to effective handling, but making observations from an impartial indicate of view helps round out what the patient told you.
The objective portion of Lather notes relates to how the trunk functions and evaluates neurological performance with the Mental Status Exam.
What observations tin can you make about the individual? Write them down as factually as possible.
The Objective phase is concerned only with raw data, non conclusions or diagnoses on your part. Record any measurable data during the client's session, including applicative test scores.
Documenting the Objective phase brings up the issue of separating symptoms from signs. Symptoms are the patient's own feel of their status, whereas signs are objective observations related to symptoms.
If a client reports having symptoms of anxiety, such as panic attacks, signs of that anxiety might include visible trembling or clenching of muscles equally well as hypertension adamant past a physical exam.
Y'all have a express window for test, so information technology'southward important to actively look for any signs that complement or contradict information given in the subjective section of the notes.
three. Assessment
Both the Subjective and Objective elements previously recorded come into result in the Assessment phase. You will certificate your impressions and brand interpretations based on the information you've gathered.
For an initial visit, the Assessment portion of your notes may or may not include a diagnosis based on the type and severity of symptoms reported and signs observed.
For common conditions such equally depression, the Cess is fairly straightforward and can often lead to a diagnosis in the offset visit or two.
For rarer and more complex conditions or those that appear co-morbidly, you may need more fourth dimension to gather information on the Subjective and Objective levels before arriving at a diagnosis.
For follow-up visits, the Assessment portion of SOAP notes covers an evaluation of how the client is progressing toward established handling goals. The Assessment volition inform your current treatment course as well as future plans, depending on whether the patient is responding to treatment as expected.
It'south essential to reflect on whether your client is showing improvement, maintaining improvements already made, worsening, or demonstrating patterns of remissions.
Similar the other sections of SOAP notes, your Assessment should just contain every bit much information as is necessary. Some Assessments will be significantly longer than others, based on the complexity of the patient's condition.
Sometimes this section of your notes will incorporate only a few snippets of information like, "Patient is sleeping ameliorate, no change in the incidence of panic attacks."
In other situations, at that place are more pieces to evaluate and your Assessment portion of notes should extend to include all the appropriate information.
4. Plan
This is where the previous three sections all come together to aid you lot determine the class of hereafter treatment. The Plan department of your SOAP notes should contain data on:
- The treatment administered in today's session and your rationale for administering it
- The client's firsthand response to the handling
- When the patient is scheduled to render
- Any instructions you gave the client
- Goals and issue measures for new problems or bug existence re-assessed
Your Programme notes should include actionable items for each diagnosis.
If your client is experiencing multiple conditions, such as mail-traumatic stress disorder (PTSD) in combination with a substance utilize disorder, your notes should include divide plans for each condition.
The goal of this department is to address all the specific deficits listed in the Assessment. When washed efficiently, the Programme sets a clear roadmap for the patient's continuing treatment and provides a window of insight for other clinicians to continue that treatment if need be.
The Plan should be consulted on each new visit, and adapted regularly based on the findings in the Assessment section.
Soap Notes in ICANotes
ICANotes is a behavioral health EHR that provides everything you demand to create SOAP notes with ease and accurateness.
With our menu-driven templates, y'all can create a clinically significant psychotherapy note inmerely iii minutes with hardly any typing.
Our system is highly intuitive and easy to pick upward and comes with the ability to create your own templates in addition to using our clinically-geared variety.
Check out a sample Soap notation that was created using ICANotes, so schedule a demo to see our powerful system for yourself.
Why Soap Notes are an Important Tool
SOAP is the about common format used by medical and behavioral health professionals, and for good reason. Since its evolution in the 1960s, the SOAP framework has been useful enough for health professionals of all stripes to implement it.
Of the many benefits SOAP provides, here are three of the nigh prominent.
![]()
Connectivity
![]()
Accuracy
![]()
Efficacy
1. Connectivity
Adoption of EHR systems is on the rise, with 89.6 percent of primary intendance providers and 61.three percent of psychiatric practices using some course of an electronic record. EHRs make integrated care possible by allowing medical and behavioral health professionals to access each other'due south notes on patients.
Using the SOAP framework enables practitioners of all specialties to communicate in a streamlined mode, providing better care for each patient.
2. Accuracy
When health care providers are not using the same framework for notes, it'due south easy for disquisitional data to get lost in translation when the next provider accesses the information. SOAP notes emphasize clarity and concision, which helps get every provider on the same folio with minimal defoliation.
The clear structure of Soap notes also increases the accuracy of your notes in general. Rather than trying to remember everything that happens in an appointment and jotting it down stream-of-consciousness style, SOAP notes requite you a way to construction your appointments to get the right information at the right fourth dimension, making it easier to think and accurately input all the necessary notes.
three. Efficacy
SOAP notes help support your end goal of providing the virtually effective care and handling for your clients. The focus on Cess and Program keeps progress at the forefront of your sessions and offers a history of efficacy you can evaluate to see what's working and what isn't.
Soap notes also create a paper trail of documentation that may be useful in the example of a malpractice suit. More than commonly, mental health SOAP notes are required for insurance reimbursements in the instance of a third-political party audit. Switching to this annotation-taking technique is better for both your patients and your practice.
Lather Notes Webinar
We cover everything you need to know on how to create better SOAP Notes in this powerful on-need webinar. Check information technology out if y'all're ready to meliorate your notation-writing!
Examples of Lather Notes
The Lather framework tin can exist incorporated into any notes taken in a behavioral health care setting. To help y'all envision the means you lot can integrate SOAP notes into your practice, here are 3 situations in which the Lather arroyo can clarify and simplify your documentation.
1. Psychiatry
You're treating a patient at an outpatient psychiatric clinic. Nosotros'll telephone call her Mrs. D. You diagnosed her with Alzheimer's, dementia, and depression three months ago, and it'southward fourth dimension for another follow-up appointment. To write her notes in the SOAP framework, y'all would follow these steps.
- Get together subjective information from the patient on her depression symptoms.
- Review lab exam results to get together data on signs of the condition and compliance with the medication regimen.
- Review notes from the final visit to determine how Mrs. D is progressing with her treatment and evaluate whether her symptoms are getting better or worse.
- Based on her progression or lack thereof, you can decide whether to accommodate her medication or make another amending to her treatment program.
In this example, Mrs. D is displaying signs of a worsening status. The Subjective investigation reveals that her depressive symptoms have not abated, and she has been having outbursts of anger. Her daughter also reports that she has had trouble sleeping.
On the Objective cease, you lot observe that her voice communication is loud and garbled, she has problem naming objects, and she expresses inappropriate episodes of rage. She also cannot perform simple arithmetic calculations and is disoriented when it comes to appointment and location.
Your Cess finds that she is non making progress on the electric current course of treatment, and you find that information technology may be appropriate to alter her Programme going forrard.
2. Individual Therapy
As medications and lab tests are not regular components of individual therapy, SOAP notes are even simpler to certificate.
In this case, we'll imagine treating a patient called Ms. P, who suffers from full general anxiety, borderline personality disorder, and major depressive disorder.
Following the steps from the example above, Ms. P's Lather notes might look like a longer version of this:
- Subjective:The patient states, "I feel amend today. I recollect my depression is improving. The therapy is helping."
- Objective:Compliance with medication is good. Relationships are reduced. Work operation is marginal. The patient has maintained sobriety. Her weight is stable, and her food and fluid intake are normal. She has reported sleep problems with difficulty falling asleep and staying comatose.
- Assessment:Ms. P appears calm, circumspect, and relaxed. There are no signs of baroque behaviors, delusions, hallucinations, or other indicators of psychosis. The patient is fully oriented. The judgment appears fair, insight into problems appears normal, and the patient did not display signs of anxiety.
- Plan:The patient will replace negative and self-defeating talk with the verbalization of realistic and positive cognitive messages.
This patient's Soap notes give a clear picture of the kind of progress she has made. In this example, the client is responding adequately well to treatment, and amending of the Plan is not necessary.
3. Group Therapy
Creating group therapy notes is necessarily more complex than documenting private sessions. You have multiple patients with multiple atmospheric condition that you have to keep rail of, making it even more crucial to exist succinct and precise in your notes. Each individual should have their own notes from each group therapy session, using the Lather format.
Each individualized group therapy note should also include the grouping blazon, the agenda for that session, the group members present, and the interventions facilitated by the grouping leader.
Creating individualized Lather notes for group therapy can be somewhat fourth dimension-consuming, merely is essential for monitoring progress over time.
SOAP Notes in ICANotes
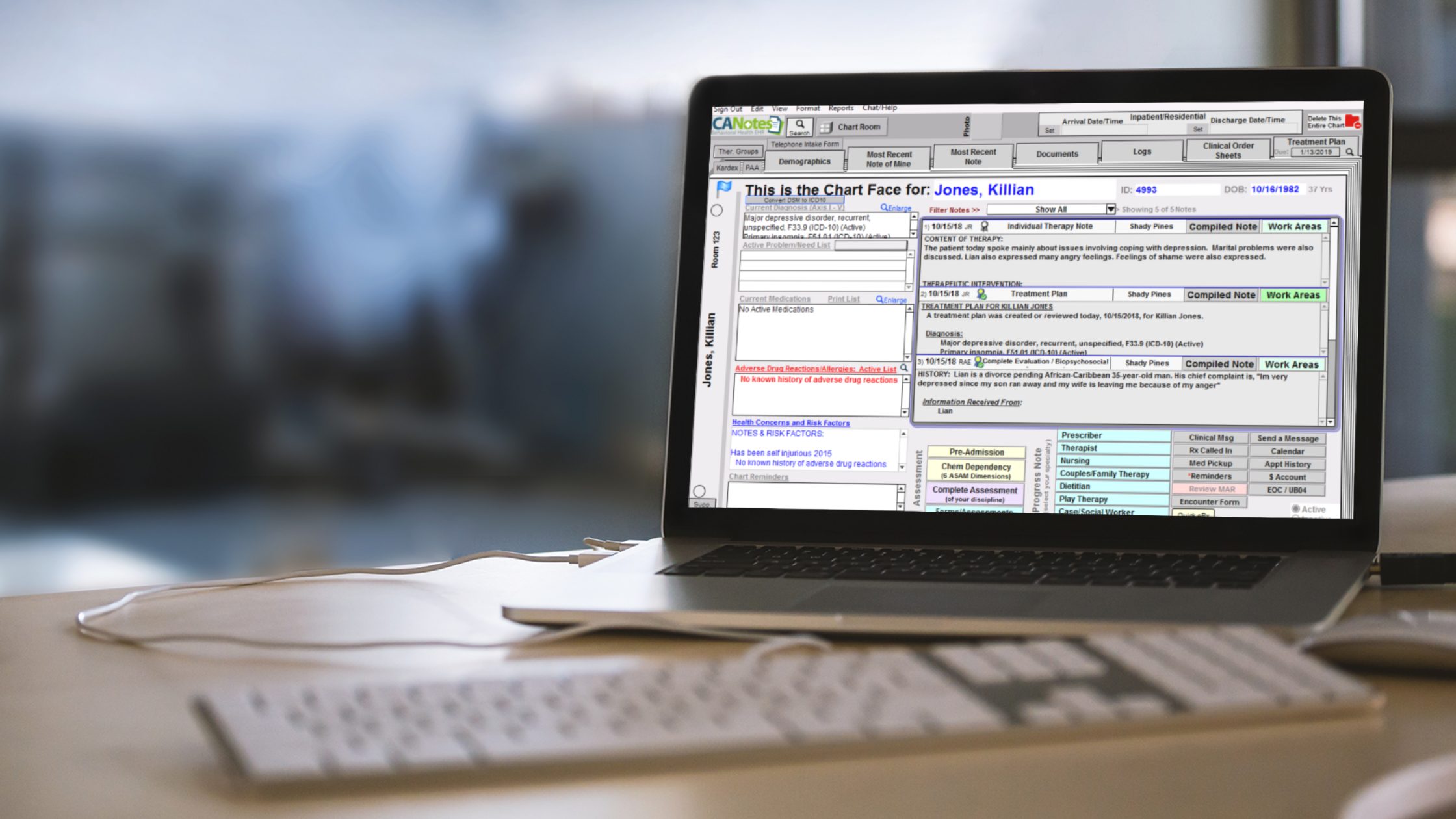
The main drawback to Lather notes is that they can oftentimes be tiresome to create. EHRs geared toward medical professionals merely don't cut it for behavioral wellness specialists, and don't offer the features clinicians need to create effective mental health Soap notes.
With ICANotes, you'll spend less time creating ameliorate documentation. Curious to see how information technology works? Annals for alive demo of our platform, or claim a complimentary trial to use the arrangement for yourself.
Higher-quality Soap notes don't have to require harder work on your role. ICANotes is proud to provide behavioral health professionals with an EHR that understands your documentation needs.
Source: https://www.icanotes.com/2018/04/25/tips-for-writing-better-mental-health-soap-notes/
Post a Comment for "Families Disclosure of Mental Illness Soap Note Example."